Within the past decade, medical research has been a burgeoning field with new understandings and innovations. One of these new medical developments includes stem cell research, which has the possibility to cure diseases such as Alzheimer’s, repair damaged tissue through regenerative medicine, and test drugs without the use of animal testing.
Yet, despite the possibilities, many people are against stem cell research because of the use of embryonic stem cells in some research. However, stem cell research has the possibility of curing diseases that we never thought could be cured, and saving thousands of lives worldwide.
What are stem cells?
Stem cell research often receives a lot of media coverage, but what exactly are stem cells? Within your body, you have many different types of cells with specific cell functions. These specialized cells can only perform certain functions and can’t turn into a different type of cell, but there is a different type of cell called stem cells.
Stem cells have three qualities that make it different from normal cells: The ability to differenciate and turn into specialized cells, the ability to divide and renew itself, and it is an unspecialized cell that cannot do specific functions of the body.
Stem cells are classified by cell potency, which is a cell’s ability to differentiate into a different cell type. Totipotent stem cells are cells that have the ability to turn into all of the cell types of the body including the extra-embryonic tissue such as the placenta. These include a zygote, which is a fertilized egg. Pluripotent stem cells can give rise to all of the cells of the body, with the exception of the placenta, and an example of pluripotent stem cells include embryonic stem cells and induced pluripotent stem cells (iPS cells). Multipotent stem cells are more limited than pluripotent stem cells, but can still differenciate into more than one, and these include adult stem cells and mesenchymal stem cells. Unipotent stem cells, such as muscle cells, can only differenciate into one cell type, although they can self-renew.
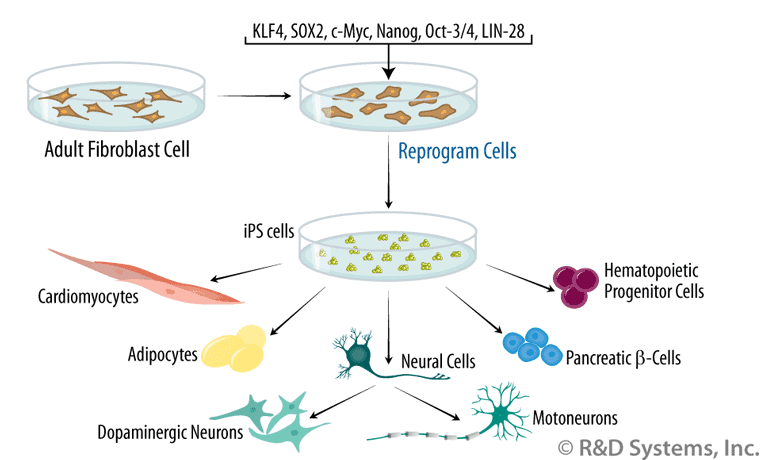
How does cell differenciation occur and what are iPS cells?
By adding growth factors, scientists can change the cell morphology, membrane potential, metabolic activity, and more to differenciate stem cells. Normally, stem cell differentiation is highly regulated by signalling pathways and modifications in gene expression to commit a cell to a lineage. Differenciation first occurs when stem cells start to differentiate into germ layers, which are the ectoderm, which gives rise to nervous tissue, hair, and skin, the mesoderm, which gives rise to blood, muscle, bone, cartilage, and other supporting structures, and the endoderm, which gives rise to the pancreas, liver, and other internal organs.
In 2007, Shinya Yamanaka revolutionized stem cell research when he discovered induced pluripotent stem cells (iPS cells). He introduced combination of transcription factor genes, specifically Oct3/4, Sox2, Klf4 and c-Myc, into mouse skin fibroblast cells through retrovirus transfection, and isolated the first induced pluripotent stem cell line that resembled embryonic stem cells. He found that by injecting the iPS cells into the blastocysts of normal mice embryos, the cells could contribute to all of the cells of the body. This made a mark on the scientific community, as previously, pluripotent stem cells could only be obtained through embryonic stem cells, which is often frowned upon by the public because of the ethical concerns of using embryos for research. Embryonic stem cells could also cause an immune response in patients, so iPS cells provided the possibility to turn somatic cells from the patient into patient-specfic iPS cells that could potentially eliminate the risk of an immune reaction. However, iPS cells aren’t completely risk-free. Some concerns currently faced by scientists include the possibility of iPS cells turning into cancer cells because of its ability to self-renew, difficulting and low-efficiency of maintaining cell lines, and since many iPS cells retain an “epigenetic memory,” these cells may have chemical signs in their DNA indicate their original cell type that make them a bit different from embryonic stem cells.
Yet, despite the challenges in stem cell research, it has huge possibilities for the future of disease. For example, according to a paper titled Controlled differenciation of stem cells, “ES cell lines with genetic disease markers have been generated through nuclear transfer technology to study the underlying cause of disease and diseases progression. Pluripotent stem cells could also be used in drug development, screening, and toxicology…Perhaps the most exciting of all applications of stem cells could be their use in cell replacement therapies and regenerative medicine.” Currently, the most popular stem cell therapy is hematopoietic stem cell transplantation, commonly known as bone marrow transplant. This therapy occurs when the multipotent stem cells from the patient, donor, or identical twin’s bone marrow, blood, or umbilical cord blood are taken and transplanted into the patient to turn into healthy blood cells to treat diseases such as leukemia or anemia. However, this procedure has many life-threatening complications and risks associated with it, including a disease called graft-versus-host disease (GVHD), which happens when the stem cells are from a donor, causing the patient’s immune system to attack the donor’s cells, and sourcing hematopoietic stem cells is often a difficult and invasive process. iPS cells could possibly eliminate the risk of GVHD and increase the number of cells available for transplant, which improves the success rate of the procedure.
“ES cell lines with genetic disease markers have been generated through nuclear transfer technology to study the underlying cause of disease and diseases progression. Pluripotent stem cells could also be used in drug development, screening, and toxicology…Perhaps the most exciting of all applications of stem cells could be their use in cell replacement therapies and regenerative medicine.”
Nathaniel S. Hwang et. al. 2007
In addition, stem cells could possibly eliminate the need for animal testing, as they could help test for toxicity and identify new therapies. To illustrate, according to an article published in the Nature journal, “Minger and his team at GE Healthcare assessed the heart cells in a blind trial against a set of unnamed drug compounds to see if the cells would reveal which compounds were toxic. When the compounds were unmasked, Minger says, they found that the cells had been affected by the known toxic compounds. But, crucially, in a number of cases, the cells identified a problem that had only been discovered after the drugs had reached the market — and after they had been approved by agencies such as the US Food and Drug Administration (FDA).”
Often times, drugs that do well in animal models do not have the same results in human clinical trials, so stem cells could help test for toxicity and screen for dangerous side effects before the drugs reach the market. This helps save time and resources, as drugs sometimes progress through clinical trial stages only to find dangerous side effects far into the develoopment process or when it has reached the market. Stem cells have been shown to have great potential to become an in-vitro model for human diseases, which allows scientists to test drugs and discoveries using cells instead of living organisms, and many pharmaceutical companies are purchasing stem cells to develop and test drugs.
“Minger and his team at GE Healthcare assessed the heart cells in a blind trial against a set of unnamed drug compounds to see if the cells would reveal which compounds were toxic. When the compounds were unmasked, Minger says, they found that the cells had been affected by the known toxic compounds. But, crucially, in a number of cases, the cells identified a problem that had only been discovered after the drugs had reached the market — and after they had been approved by agencies such as the US Food and Drug Administration (FDA).”
Daniel Cressey, science journalist for Nature journal
However, when people think of stem cell therapy, most people think of regenerative medicine. Stem cell research in regenerative medicine uses embryonic, adult, or iPS cells to revive or replace damaged tissue, as diseases such as Parkinson’s, Type 1 diabetes, neurodegenerative diseases, macular degeneration, or coronary disease cause tissue damage, and stem cell therapy can help generate new, healthy tissue by inducing stem cells to differenciate into a specialized tissue as scientists begin to understand stem cell development, differenciation, and maintenance.
It is estimated that around one in three Americans could benefit from regenerative medicine, as stem cell therapy could help replace damaged tissue or help the body’s repair system to heal tissues or organs. These therapies include cell therapy, which is the injection of stem cells into the body, immunomodulation therapy, which helps regeneration by injecting stem cells, and tissue engineering, which involves growing tissues or organs in a lab and transplanting it to a patient.
Scientists have been using cord blood stem cells to slow the loss of insulin production in diabetic children, repair damaged cardiac and nervous tissue, and more, as the field of regenerative medicine is very promising. Particularly, neurodegenerative diseases such as Parkinson’s, Alzheimer’s, and Huntington’s Disease that we currently think of as incurable today could potentially be cured with stem cell therapy, with scientists discovering neural stem cells, proving that neurons can be regenerated. When mice were injected with neural stem cells, researchers found that the mice had increased cognitive ability. While turning skin biopsies into neural stem cells through iPSC technology is still a relatively new development, stem cell research could one day treat for those suffering from neurodegenerative diseases. With millions of people suffering from diseases worldwide, stem cell research provides a promising future in regenerative medicine, drug safety, organ transplants, and more. While there have been risks associated with stem cell therapies, scientists are hopeful that one day, stem cell research will be able to save millions of lives and improve medical technology for all.
“Without a doubt, stem cell research will lead to the dramatic improvement in the human condition and will benefit millions of people.”
Eli Broad, entrepreneur and philanthropist
Bibliography
Zakrzewski, W., Dobrzyński, M., Szymonowicz, M. et al. Stem cells: past, present, and future. Stem Cell Res Ther10, 68 (2019). https://doi.org/10.1186/s13287-019-1165-5
*Note: This paper goes into depth about what stem cells are and the types of stem cell treatments, I would recommend reading it if you’re interested in stem cell research!
Stem Cells. 14 May 2020, medlineplus.gov/stemcells.html.
“What Is the Difference between Totipotent, Pluripotent, and Multipotent?” What Is the Difference between Totipotent, Pluripotent, and Multipotent? | NYSTEM, stemcell.ny.gov/faqs/what-difference-between-totipotent-pluripotent-and-multipotent.
Hildreth, Cade. “Do You Know the 5 Types of Stem Cells?” BioInformant, 3 Aug. 2019, bioinformant.com/do-you-know-the-5-types-of-stem-cells-by-differentiation-potential/.
Murnaghan, Ian. Multipotent Stem Cells, 5 Sept. 2019, www.explorestemcells.co.uk/multipotentstemcells.html.
“Stem Cell Differentiation.” Tocris Bioscience, www.tocris.com/cell-biology/stem-cell-differentiation.
“Bone Marrow Transplant.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 24 Oct. 2019, www.mayoclinic.org/tests-procedures/bone-marrow-transplant/about/pac-20384854.
“Regenerative Medicine.” AABB, AABB, www.aabb.org/aabbcct/therapyfacts/Pages/regenerative.aspx.
Yee, J. (2010) Turning Somatic Cells into Pluripotent Stem Cells. Nature Education3(9):25
Cressey, Daniel. “Stem Cells Take Root in Drug Development.” Nature, 2012, doi:10.1038/nature.2012.10713.
Scudellari, Megan. “How IPS Cells Changed the World.” Nature, vol. 534, no. 7607, 15 June 2016, pp. 310–312., doi:10.1038/534310a.
Wuputra, K., Ku, C., Wu, D. et al. Prevention of tumor risk associated with the reprogramming of human pluripotent stem cells. J Exp Clin Cancer Res39, 100 (2020). https://doi.org/10.1186/s13046-020-01584-0
Singh, Vimal K et al. “Describing the Stem Cell Potency: The Various Methods of Functional Assessment and In silico Diagnostics.” Frontiers in cell and developmental biology vol. 4 134. 22 Nov. 2016, doi:10.3389/fcell.2016.00134
Hwang, Nathaniel S et al. “Controlled differentiation of stem cells.” Advanced drug delivery reviews vol. 60,2 (2008): 199-214. doi:10.1016/j.addr.2007.08.036



